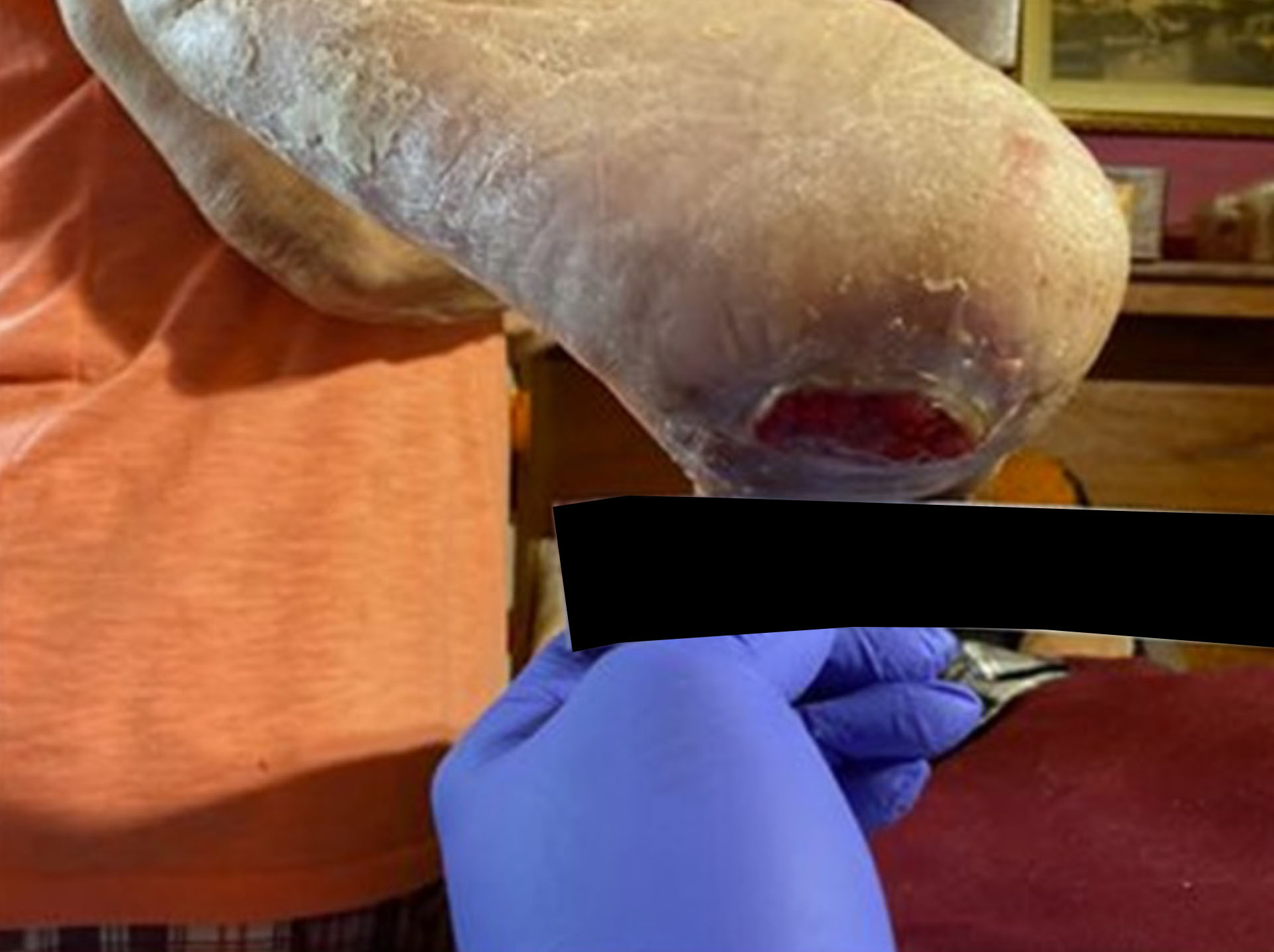
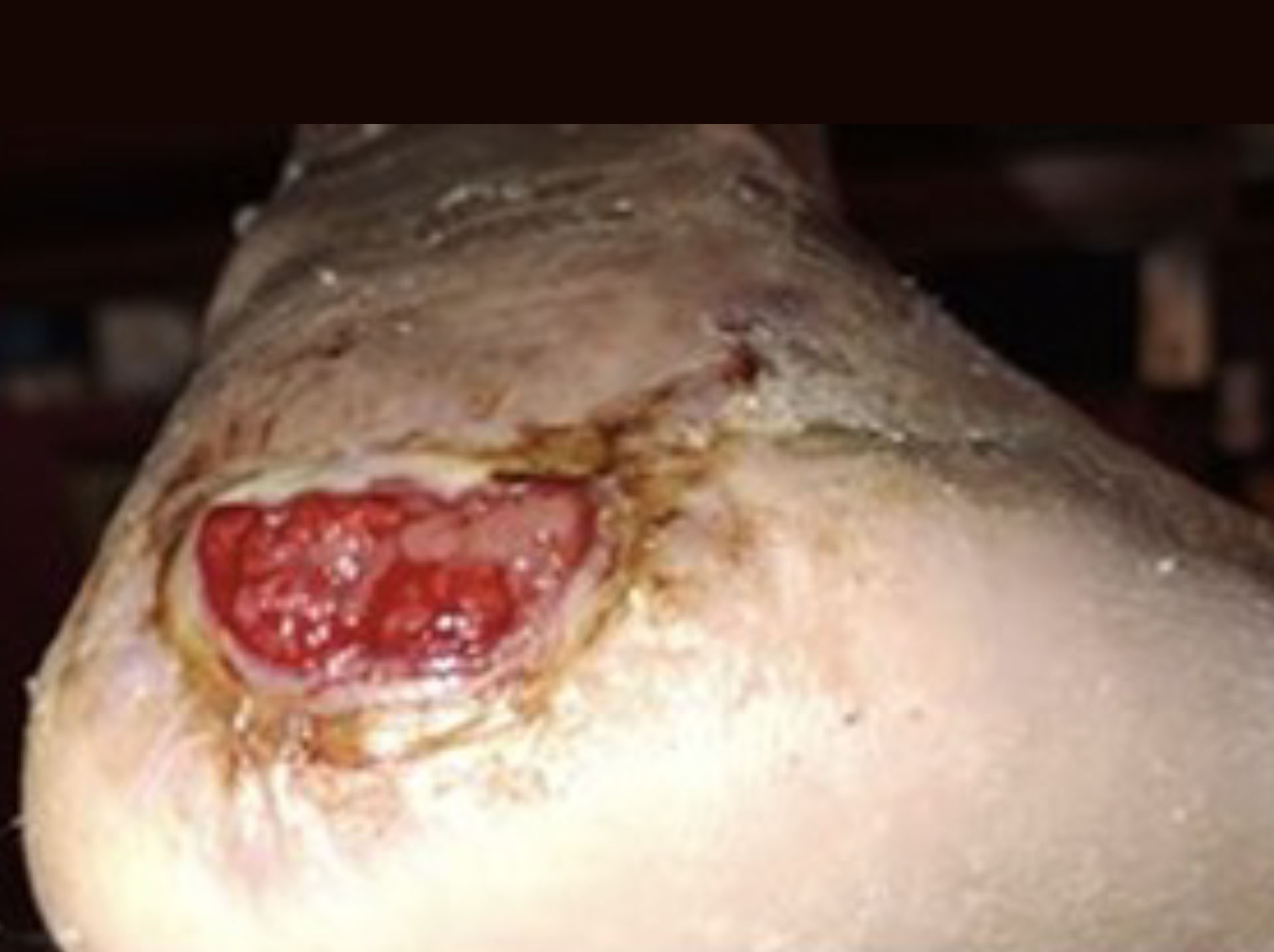
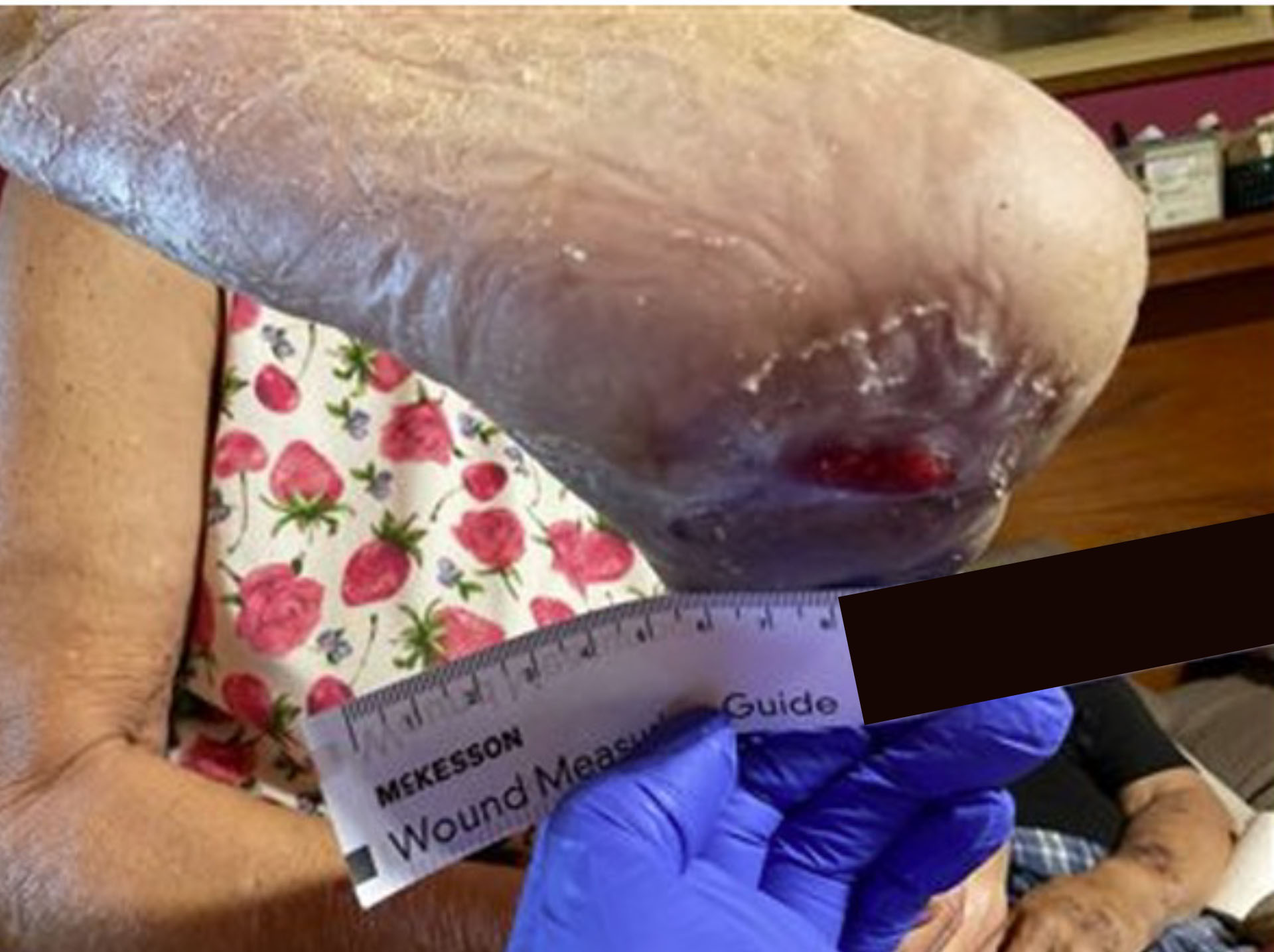
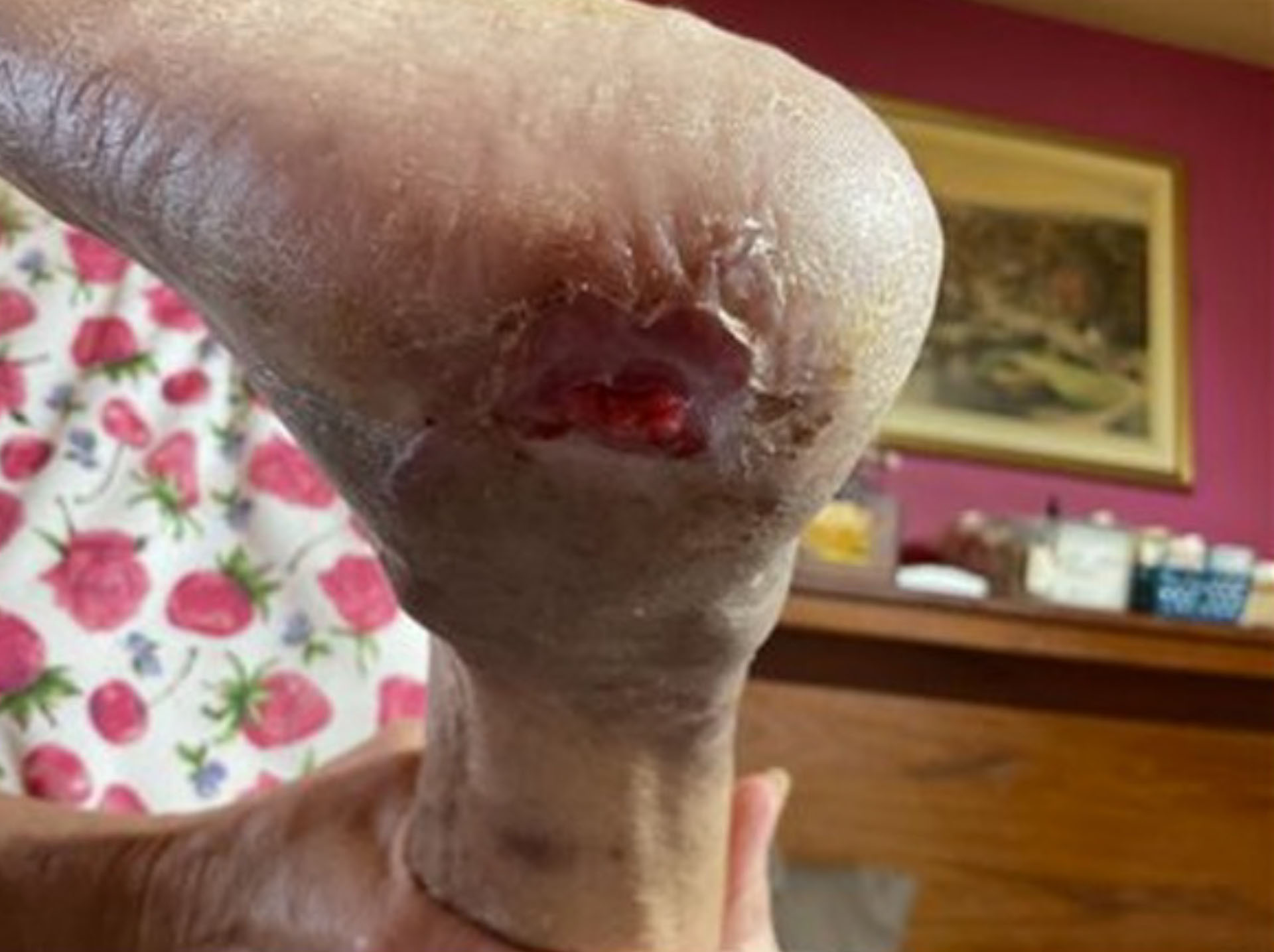
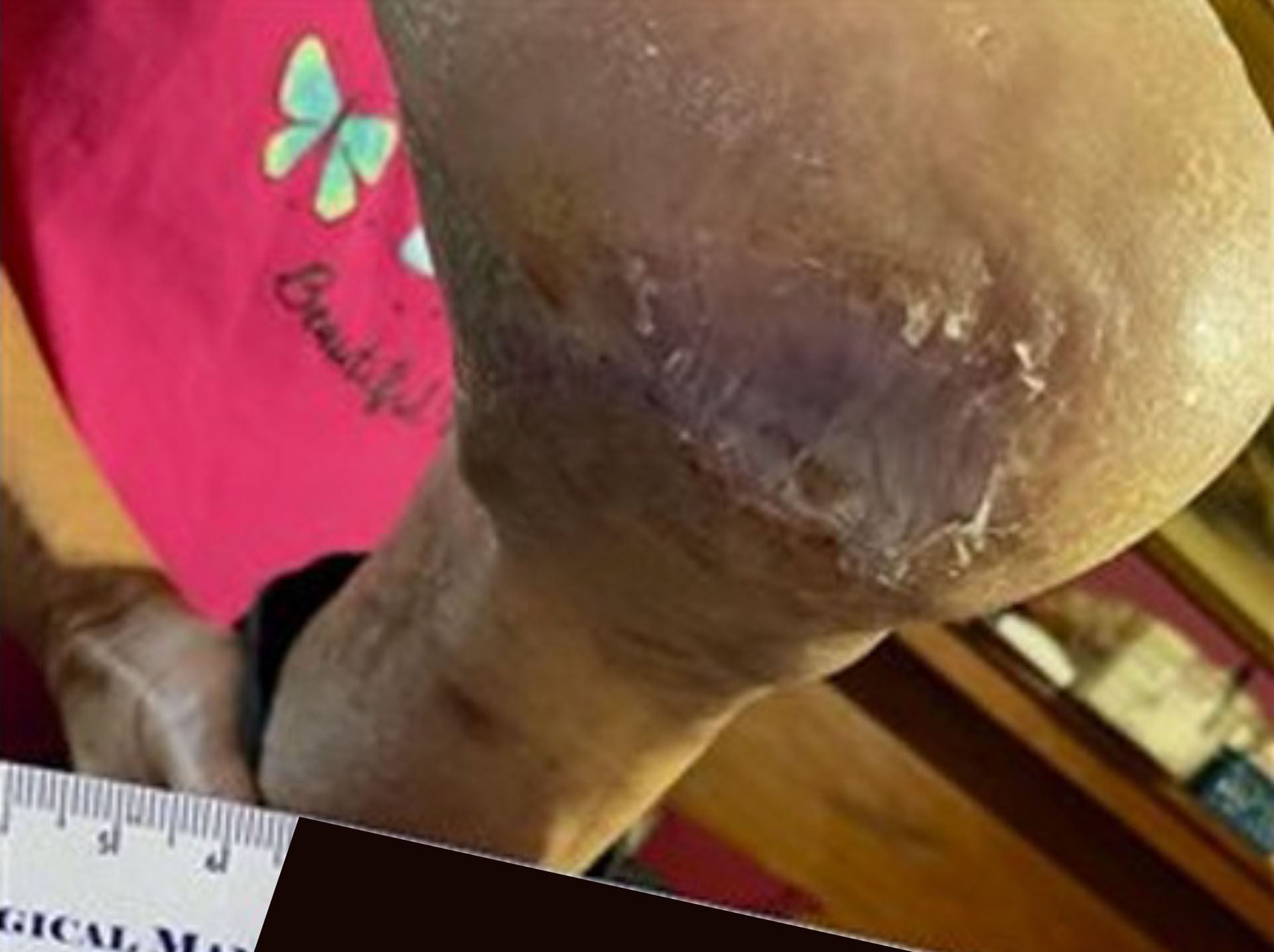
Stage 3 Heel Pressure Ulcer –Treated with DermaBind FM
Patient Overview
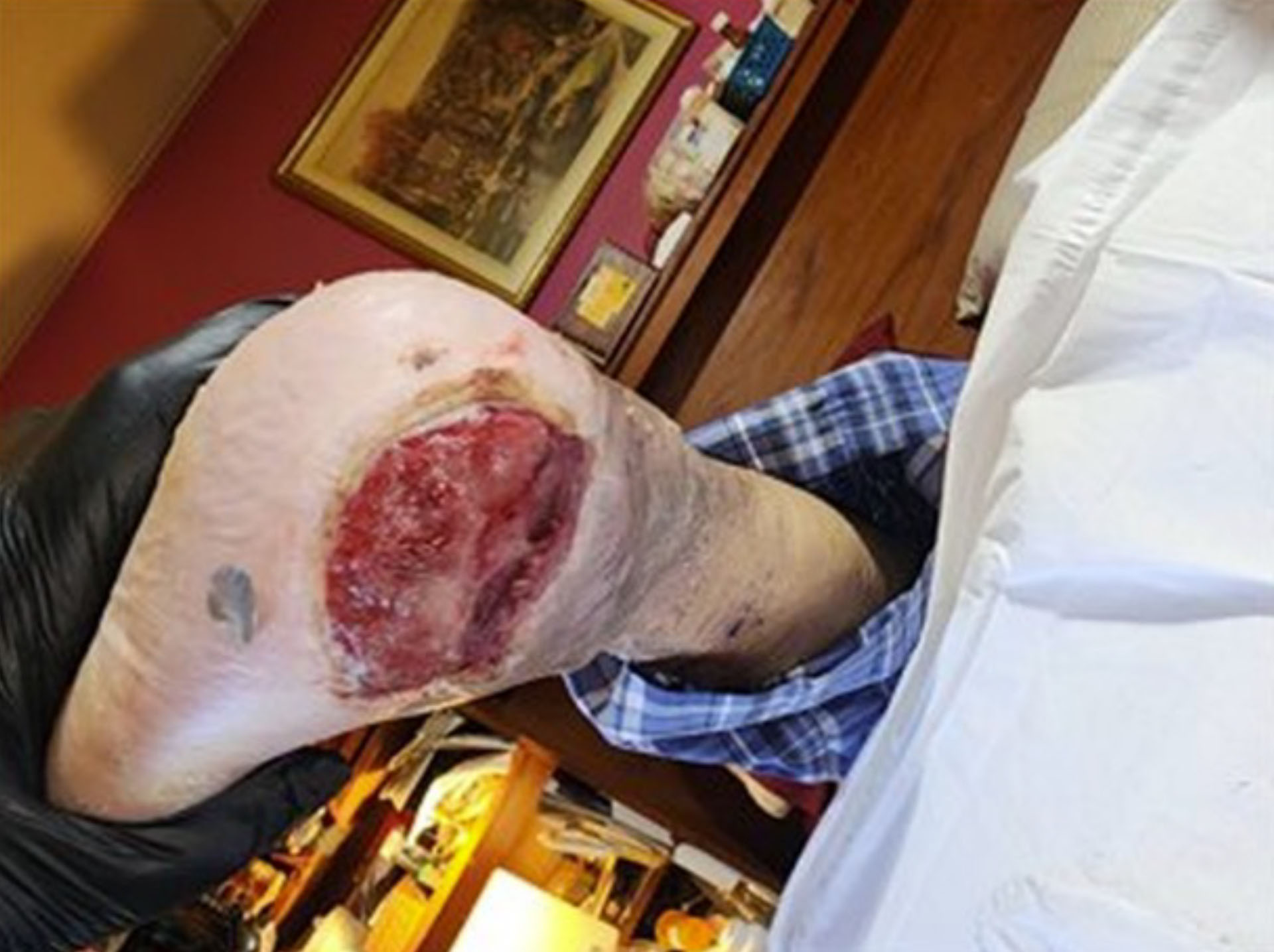
A 68-year-old male with a complex medical history, including end-stage renal disease (ESRD), mixed hyperlipidemia, hypothyroidism, chronic pain syndrome, and a history of cigar smoking, became wheelchair dependent following a recent aortic valve replacement and subsequent skilled nursing facility rehabilitation. In April 2025, while self-propelling his wheelchair, the patient developed a Stage 3 pressure ulcer on his right heel. He presented on 6/18/25 with an eight-week-old, non-healing ulcer.
Failed Standard of Care
The patient underwent > 30 days of standard of care, which included nutritional optimization, moist wound care, infection management, serial sharp debridement, medi-honey, calcium alginate dressings and offloading. Despite these measures, the ulcer showed no evidence of healing. Due to a lack of improvement, the provider determined the wound was appropriate for advanced treatment with an allograft. Vascular studies completed but unavailable for the case study report.
Treatments:
The ulcer was cleansed throughout the course of care with Dermal Wound Cleanser, SKIN‑PREP applied initially for peri wound protection. DermaBind was applied weekly and secured with a contact layer and steri‑strips, then covered with bordered foam and a Kerlix wrap. Offloading with a heel boot was required at all times. Outer dressings could be changed if soiled, provided the contact layer remained undisturbed. As drainage decreased, outer dressings were left in place for the full week. Once the wound approached near‑complete re- epithelialization, therapy transitioned to Collagen Ag+ with foam and gauze for one additional week until full resolution.
Findings:
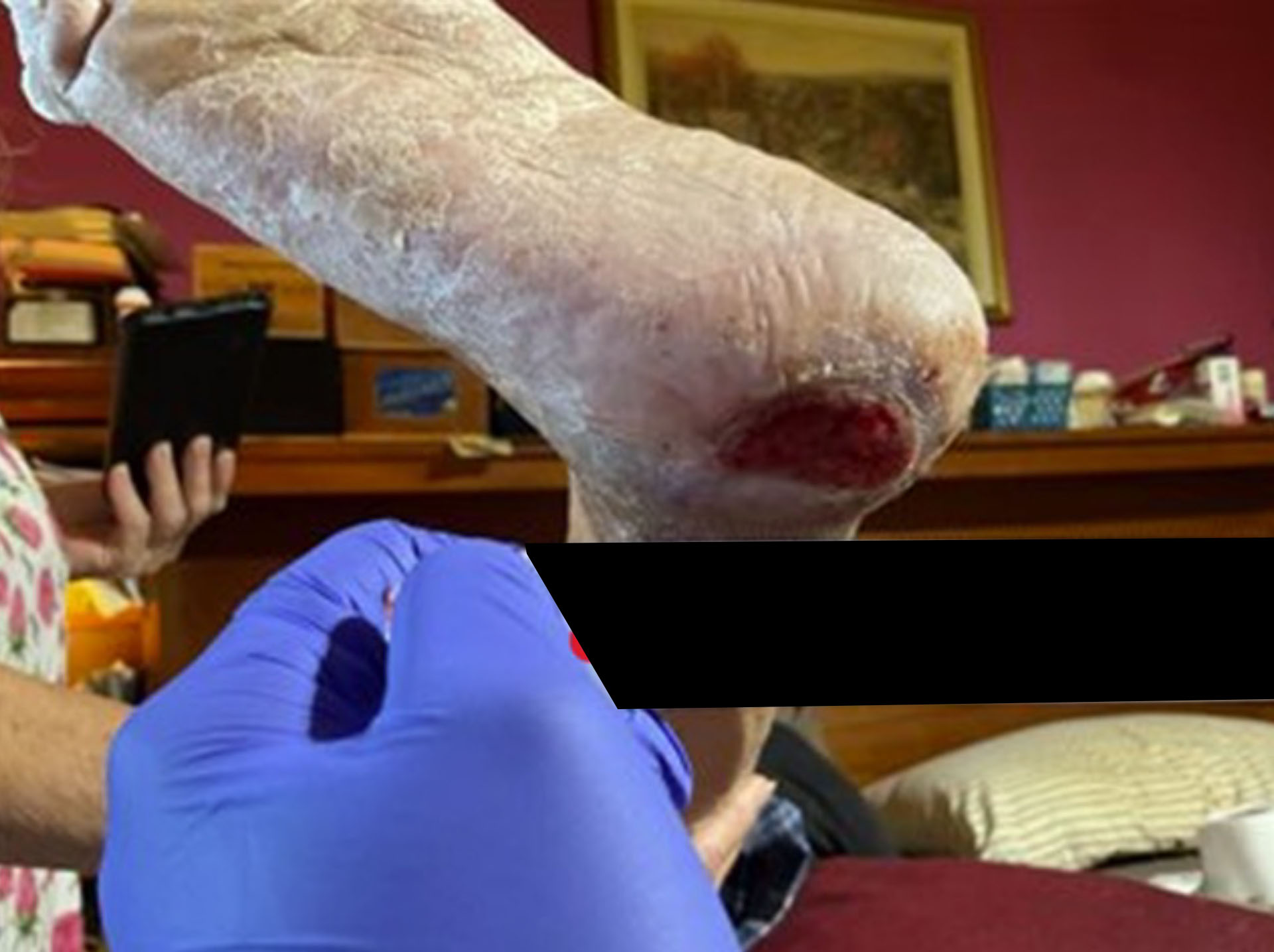
The patient underwent six allograft applications, then transitioned to standard of care for just over one week. The wound continued to progress and ultimately achieved full resolution, with 100% re‑epithelialization documented on 8/15/25.
| Date | Length cm | Width cm | Surface Area cm² | Depth cm | Volume cm³ |
|---|---|---|---|---|---|
| Allograft Application #1 (6/23/2025) | 3.7 | 5 | 18.5 | 0.3 | 5.55 |
| Allograft Application #2 (6/30/2025) | 3.2 | 4.5 | 14.4 | 0.3 | 4.32 |
| Allograft Application #3 (7/7/2025) | 2.9 | 3.2 | 9.28 | 0.3 | 2.78 |
| Allograft Application #4 (7/14/2025) | 2 | 2.9 | 5.8 | 0.2 | 1.16 |
| Allograft Application #5 (7/21/2025) | 0.9 | 2.5 | 2.25 | 0.3 | 0.67 |
| Allograft Application #6 (7/28/2025) | 0.7 | 1.9 | 1.33 | 0.2 | 0.26 |
| Transitioned to Collagen Ag+ (8/4/2025) | 0.6 | 1.2 | 0.72 | 0.2 | 0.14 |
| Observed 100% re-epithelization (8/15/2025) | 0 | 0 | 0 | 0 | 0 |

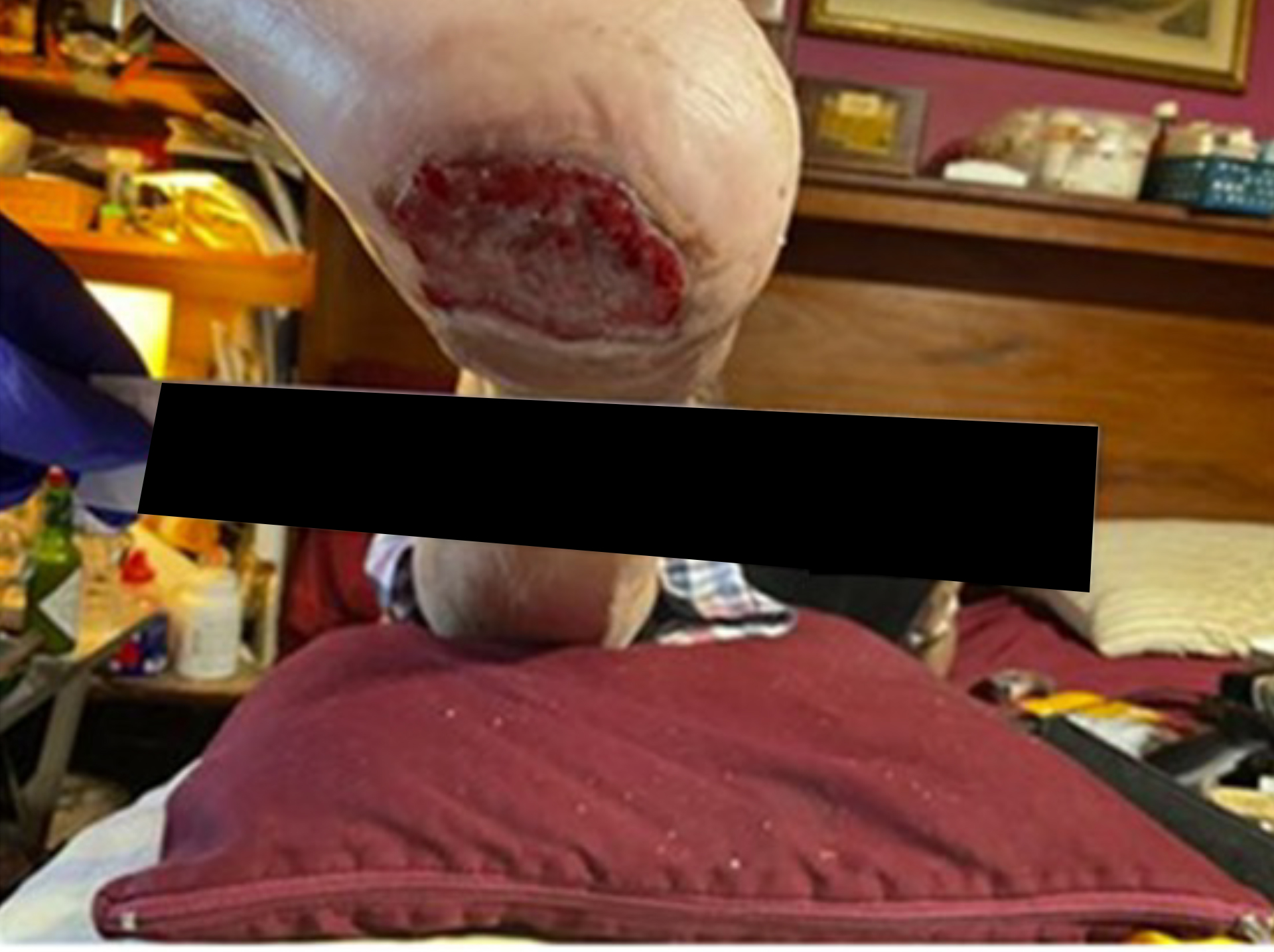
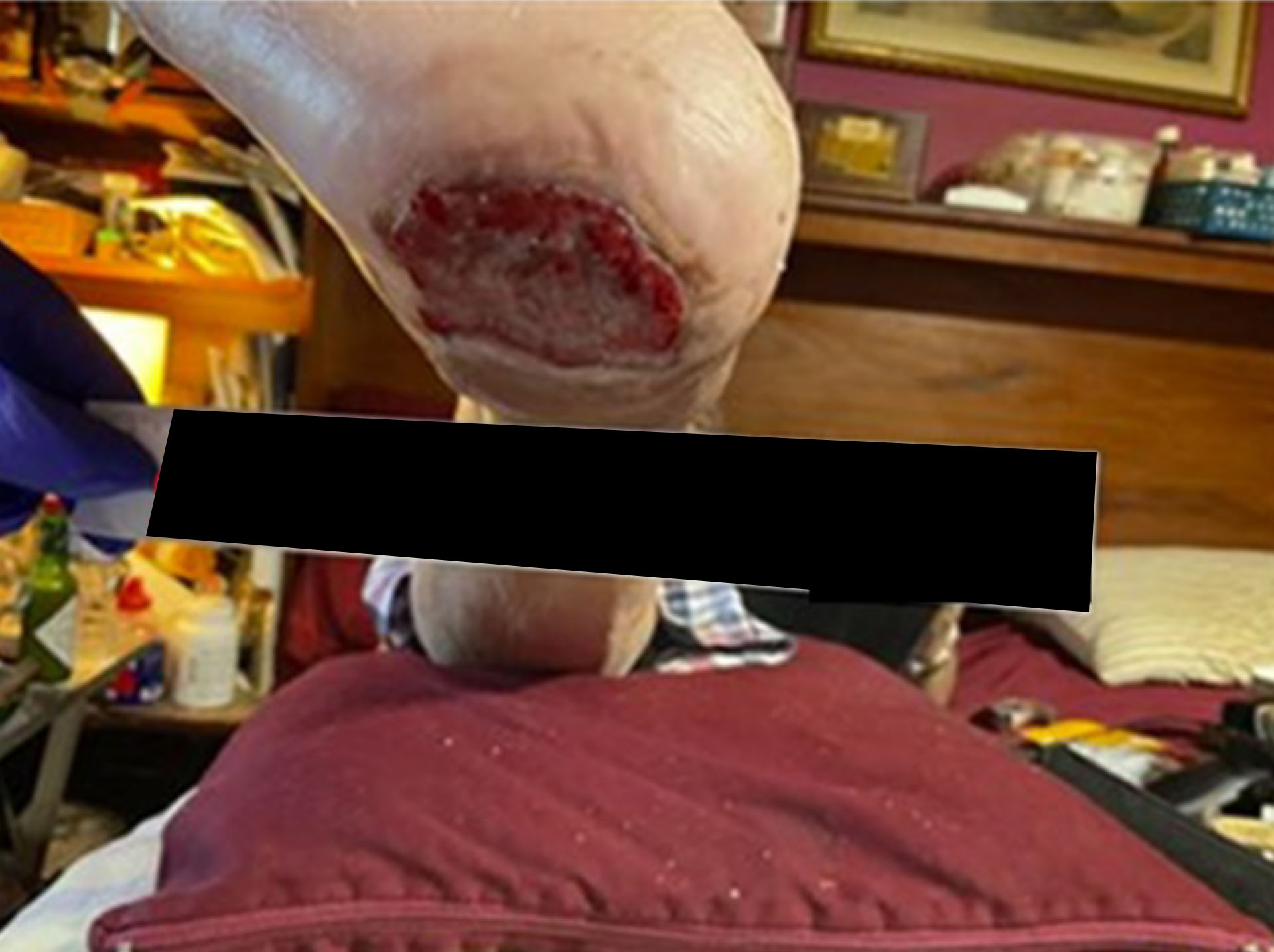
Before & After Wound Images
Ethical approval and patient consent
Institutional Review Board approval was not required for this one patient case as patient had already been treated by their provider with DermaBind based on medical necessity and failed conservative treatment. Patient consent was obtained by their provider for the use and release of deidentified data, and publication of photographs/images.
References
Mendivil, J., McMahon, A. E., Ojelade, O. T., Hobson, K., Marballie, M., Alvarez, S., Adu Aboagye, V., Chiamba, G., Gowdie, D., Landrum, W. E. II, Alzindani, A., Yazdani, H., Petty, G., Simard, M. C., Schmid, D., & Meadors, J. (2025). Clinical use of DermaBind TL/FM as a wound covering for hard to heal wounds of various aetiologies: A case series. Journal of Wound Care, 34(11). https://doi.org/10.12968/jowc.2025.0448
Provider Information
Provider Name: Willie E. Landrum II, MD, WCC